March 17, 2026
Menopause has many names: the Change, the Pause, the big M, just to name a few.
No matter what you call it, menopause is coming for you — and every other woman — somewhere around age 51, on average. Or maybe you're already on the other side.

For some women, symptoms associated with hormonal changes during perimenopause and menopause come on gradually. Others are hit hard. But most women can agree that the more noticeable effects — hot flashes, brain fog and night sweats — can take a toll.
"Women report symptoms of menopause across multiple organ systems," says Lisa Brennaman, MD, OB/GYN division director at MU Health Care. "Symptoms can range from being a minor nuisance to impacting daily life, making it difficult to function in your workplace or within family relationships."
What women don't always notice are the detrimental health effects happening below the surface — things like bone loss and increased risk of urinary tract infection (UTI). The good news is that hormone replacement therapy (HRT) can help, but it's not a one-size-fits-all solution.
Dr. Brennaman shares everything you need to know about HRT and menopause.
What's Happening With Your Hormones During Perimenopause and Menopause
The hormones we are talking about are the female sex hormones, estrogen and progesterone. The big player in menopause is estrogen, which is a broad term for a hormone group that includes:
- Estrone, the primary form of estrogen your body makes after menopause
- Estradiol, the most potent and most abundant type of estrogen produced during a woman's reproductive years
- Estriol, the most active form of estrogen during pregnancy
Hormone production begins to decrease in your mid-30s. Once you hit menopause — going a full 12 months without a menstrual period — the primary estrogen in your body changes from estradiol to estriol. In a nutshell, estrogen as you know it has officially left the building.
Progesterone — whose main job is to support pregnancy and menstruation — decreases as ovulation decreases. There are some side effects of decreased progesterone, but the biggest concern is that low levels of progesterone throw off the estrogen-progesterone balance. HRT helps reestablish that balance.
Benefits of HRT
HRT cannot completely reduce the effects of aging that take place post menopause. But it can significantly reduce the health risks associated with low estrogen.
"There are effects on our organs as a result of aging and hormone changes that even HRT
cannot completely erase or overcome," says Dr. Brennaman. "But when we study women who do not use HRT versus those who do, HRT provides a significant risk reduction in multiple areas of your health."
Benefits of HRT include:
- Alleviates common symptoms of menopause, including hot flashes, brain fog and night sweats
- Helps with genitourinary syndrome of menopause symptoms, which affect the bladder, urethra and vagina
- Reduces all-cause mortality risk, which means reducing your risk of dying from any cause, including cardiovascular disease and cancer
- Supports bone density and muscle mass to reduce the risk of osteoporosis, fractures and falls
Concerns and Risks of HRT
Personalized care is critical with HRT because of the associated risks. The risks are higher for people with certain health conditions or lifestyle factors.
HRT may increase your risk for:
- Blood clots in the legs (deep vein thrombosis) and lungs (pulmonary embolism)
- Breast cancer, in women taking estrogen and progesterone — risk is unchanged if you only take estrogen
- Endometrial cancer, if not combined with progesterone or progestin in women with a uterus
- Heart attack, if you have other risk factors, such as prior heart attack or family history of heart disease
- Stroke, if you have other risk factors such as a previous stroke
HRT is not recommended for people who have:
- Active cancer
- Active liver disease
- History of stroke or heart attack
- Uncontrolled hypertension
"Smoking is not a contraindication for HRT, but women who smoke should proceed with caution," Dr. Brennaman says. "We know that smoking amplifies the risks of HRT."
HRT Options for Menopause and Perimenopause
Your options for HRT may vary according to your symptoms and whether you have gone through menopause yet. Women who have a uterus must take a combination of estrogen and progesterone or progestin (a synthetic form of progesterone) to reduce cancer risk. If you do not have a uterus, your HRT may include only estrogen.
HRT options in perimenopause and menopause include:
Systemic Hormone Therapy
Systemic hormone therapy is absorbed into the bloodstream and affects every area of your body. It can reduce symptoms impacting your sleep, temperature, cognition and joint pain.
"Most patients notice improved symptoms within seven days," Dr. Brennaman says. "The goal is a reduction in frequency, intensity and severity. If your symptoms improve by 80%, we consider that a success."
Systemic hormone therapy can be administered in several ways, including:
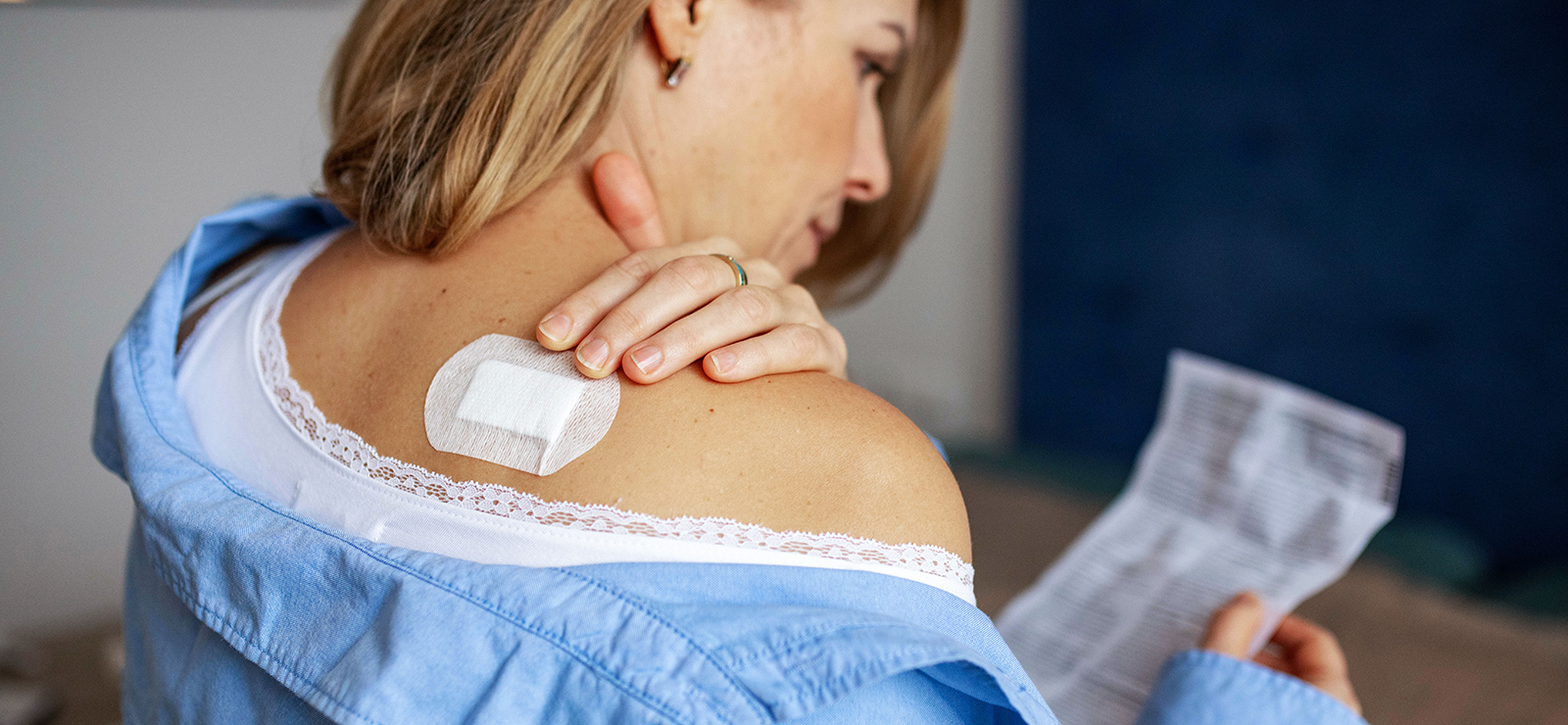
- Transdermal patch worn on your skin
- Gel, cream or spray
- Oral medication
- Vaginal ring
Since progesterone and progestin are poorly absorbed through the skin, they are typically administered as an oral capsule.
Topical Vaginal Estrogen
Topical vaginal estrogen serves a different purpose than systemic HRT. It helps with a condition called genitourinary syndrome of menopause, which involves menopause-related changes to the vagina, bladder and urethra. Symptoms include vaginal dryness, urinary urgency and postmenopausal UTIs.
Topical vaginal estrogen — which comes in a cream, vaginal tablet or vaginal ring — is a lower dosage of estrogen and does not provide the same benefits of systemic HRT. However, they are commonly used in combination.
"Topical vaginal estrogen is safe for virtually all women,” Dr. Brennaman says. "Consistent use of topical vaginal estrogen reduces the risk of postmenopausal UTI by more than 50%. Data also shows that the amount of topical vaginal estrogen absorbed by the bloodstream is negligible."
HRT in Perimenopause
Perimenopause symptoms that include menstrual irregularity can be treated with combination birth control pills. They contain a higher dose of estrogen and progestin than HRT and can provide better menstrual control than HRT used in menopause.
If your symptoms do not include menstrual issues, you can use the same HRT that is used after menopause. However, Dr. Brennaman notes that you will need periodic reassessment by your doctor to determine whether menopause occurred and to adjust HRT as you progress through the transition.
Why Timing Matters With HRT
There is no limit on how long you can use HRT based on current guidelines. Annual reevaluation helps determine if the risk versus benefit ratio changes as you age.
When you start HRT does matter. Experts recommend beginning HRT within 10 years of menopause.
"Researchers studied women who began HRT within 10 years of menopause and followed them for the next 20 years," Dr. Brennaman says. "We now know that the closer to menopause that you start taking estrogen, the safer the medications are for you."
Where to Start With HRT
If you are considering HRT, make an appointment with your primary care doctor or OB/GYN. Before the appointment, prepare by:
- Educating yourself: Dr. Brennaman recommends The Menopause Society, which provides a variety of articles and videos.
- Keeping a symptom diary: Track menopausal symptoms and menstruation, if you still get a period.
- Paying attention to your mental health: Incidence of anxiety and depression peaks during the transition through menopause and may need to be addressed and treated separately from HRT.
Don't expect your provider to order hormone testing. Most menopausal experts guide hormone therapy based predominantly on symptoms and reserve hormone testing for difficult cases.
"The symptoms of menopause are real and there is treatment available that is safe, effective and affordable," Dr. Brennaman says. "Women deserve to be listened to, and if you feel like you are not being heard or are not being offered any options, seek care from a different provider."
Next Steps and Useful Resources
- Want to speak with a doctor? Talk to a primary care or OB/GYN provider today.