May 05, 2023
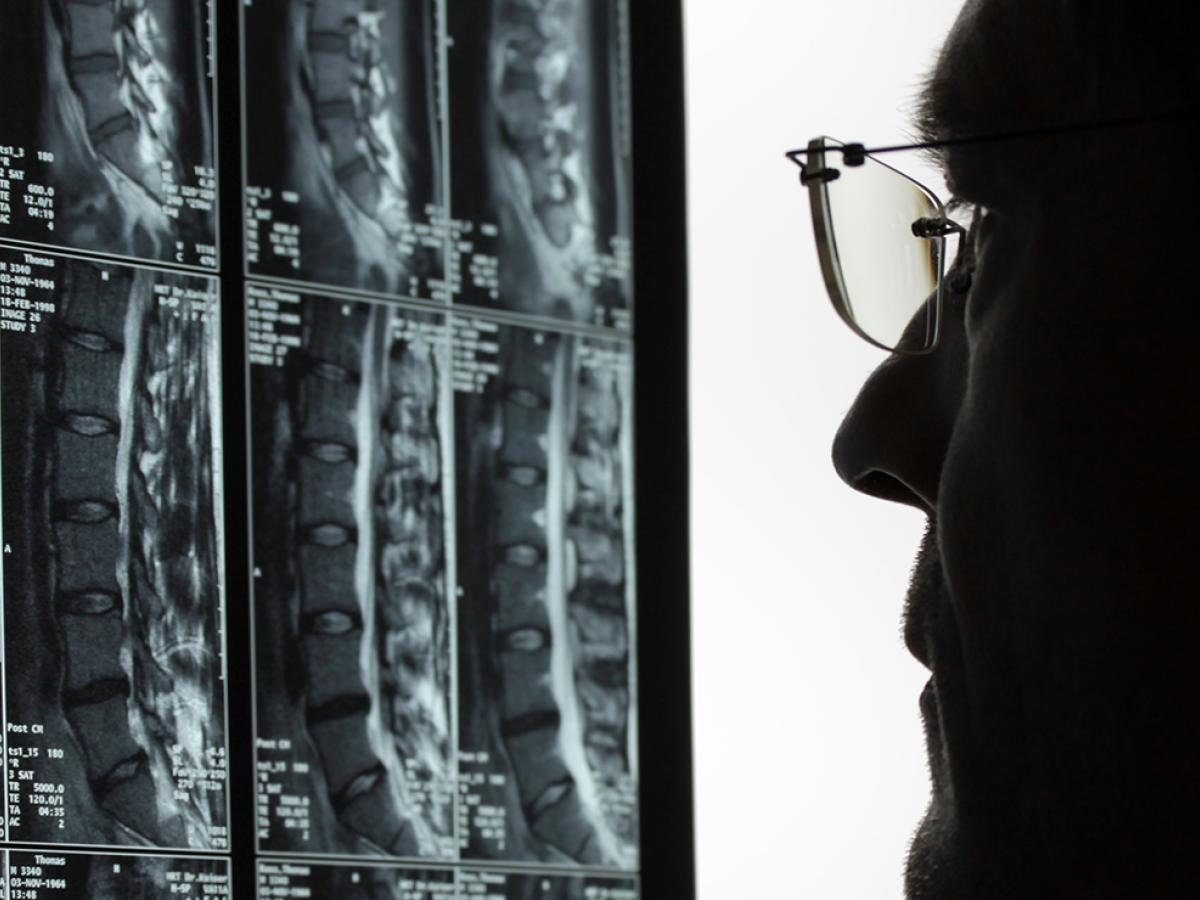
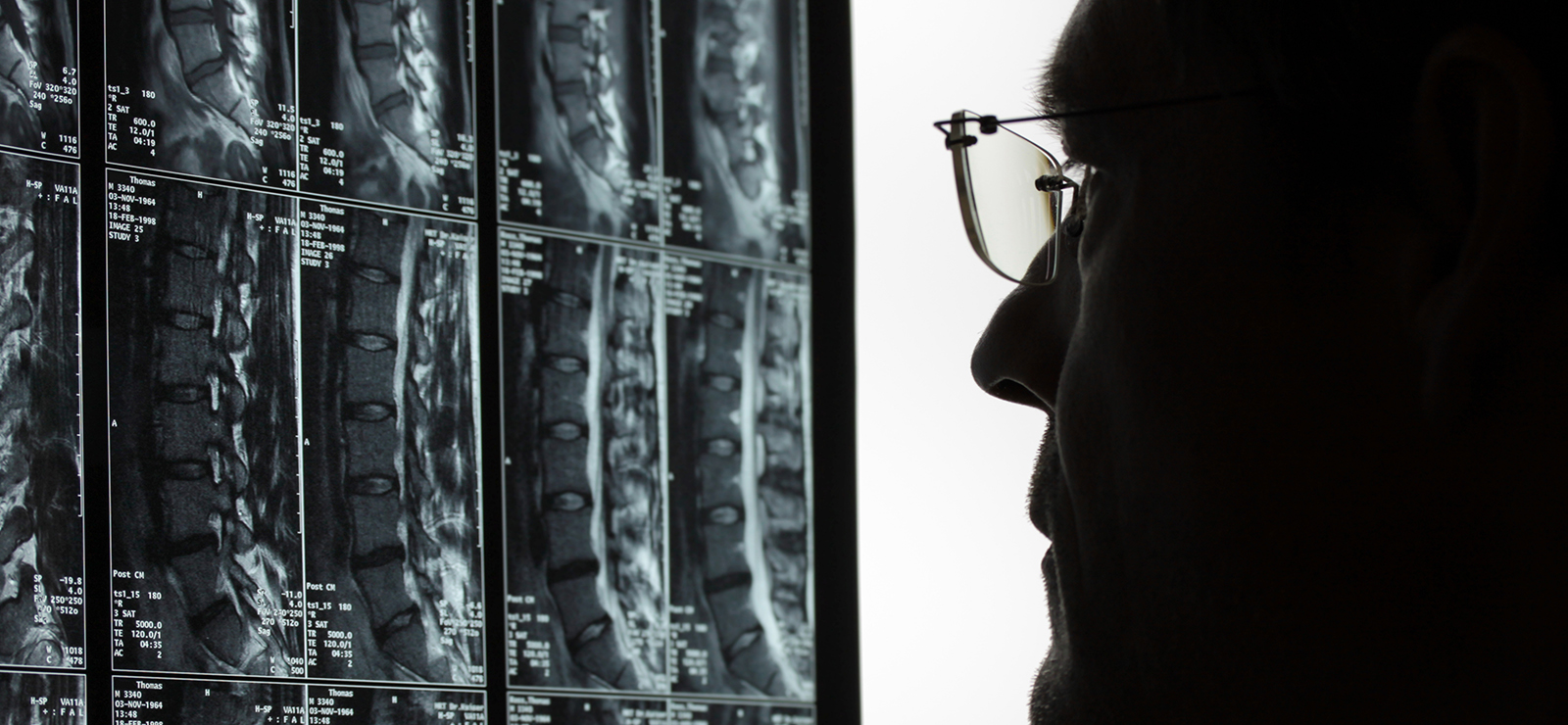
Developing new procedures is critical to advancing medicine. But innovation doesn’t happen overnight — it takes years or even decades of testing and tweaking before a procedure meets Food and Drug Administration (FDA) standards.
Only three out of 1000 school-age children have a curve measuring more than 30 degrees. But if the curvature is greater than 50 degrees, it’s more likely that the curve will get progressively worse.

Behind it all, says MU Health Care pediatric orthopaedic surgeon Dr. Daniel Hoernschemeyer, is the passion for improving care and outcomes for patients.
Dr. Hoernschemeyer should know. He spent the past 13 years helping to pioneer vertebral body tethering (VBT) and is one of only a few surgeons in the Midwest performing this procedure. This innovative surgical procedure treats idiopathic scoliosis (abnormal curvature in the spine) in growing children without fusing the bones of the spine.
“The pursuit is powered by a drive to innovate and bring something new that will be game-changing,” Dr. Hoernschemeyer says. “For me, if you can maintain a child’s flexibility, help them return to activities, and preserve the anatomy of their spine, you’ve pushed the care, the innovation and the surgeries in the right direction.”
The path to VBT’s 2019 FDA approval involved hard work, trust and a team effort — and the procedure continues to evolve. Dr. Hoernschemeyer shares a peek into the process and his journey with VBT for scoliosis:
The Promise of a Non-Fusion Treatment for Scoliosis
What is spinal tethering?
VBT is a treatment option for children with idiopathic scoliosis who still have a lot of growing to do. It uses a strong, flexible cord attached to the outside of the spine’s curve. The tether puts pressure on the outer edge of the curve while the inner part continues to grow, eventually achieving a straighter spine.
Unlike other treatments for scoliosis, the tethering device allows the spine to bend and flex. But not everyone is a candidate for the treatment. VBT may be an option for children who:
- Are skeletally immature and still have growing to do
- Have a Cobb angle (degree of curvature) of 35 to 65 degrees
- Haven’t had success, or cannot tolerate, wearing a brace
- Need surgical treatment to fix idiopathic scoliosis
Children with severe scoliosis often need surgery to improve spine curvature and prevent it from worsening. Traditionally, that surgery involves spinal fusion — realigning and then permanently connecting some of the vertebrae.
Spinal fusion can successfully improve a curved spine, but the fused area stays permanently stiff and may limit range of motion and flexibility. Spinal fusion also stops the growth of the spine. That doesn’t mean children won’t get taller after the surgery — their legs can continue to grow.
Early in his career, Dr. Hoernschemeyer studied thoracoscopic surgeries — using a small camera (called a thoracoscope) inserted through a small incision in the chest wall to gain access to the chest and thoracic (upper) spine. He loved the idea of doing spinal corrections in such a non-invasive way.
But fusing the spine still limited movement and wasn’t an ideal treatment for kids who were still growing. He looked forward to the development of non-fusion technology that could be used to treat scoliosis.
In 2010, almost a decade after his initial studies, Dr. Hoernschemeyer got his wish. A patient’s family approached him asking about a new procedure they’d heard about called vertebral body tethering, also known as spinal tethering.
“Once that technology evolved and this family brought it to my attention,” he explains, “I continued my pursuit of thoracoscopic work in the pediatric spine and chest.”
Early studies comparing VBT to spinal fusion reveal that fusion achieves greater correction more consistently than VBT — typically straightening a spinal curve to less than 25 degrees. But VBT provides greater spine flexibility, and may improve quality of life and patient satisfaction following the procedure.
Spine Tethering Surgery as an Experimental Treatment
Procedures such as VBT are often introduced as experimental before achieving FDA approval, which requires a high level of scientific proof. By 2013, there was enough evidence to support using VBT as an experimental procedure for patients. The first VBT surgery Dr. Hoernschemeyer performed required intense mental and physical preparation.
“It makes sense that you would want to keep the motion in your child's spine. But at the same time, you're learning the risks of an unknown procedure,” Dr. Hoernschemeyer says.
“We mapped it all out and spent time drawing how we wanted everything to be, down to how we’d place the equipment in the operating room,” he continues. “Now that we’ve performed plenty of surgeries over the past 10 years, it’s become a well-oiled machine.”
Improving VBT Surgery
Even after a new procedure is successfully performed as an experimental procedure, the real work is yet to come. Surgeons learn more about the procedure every time they perform it, finding ways to refine it and improve patient outcomes.
“You’re always proceeding with caution, but you’re also always looking back at what you’ve done,” Dr. Hoernschemeyer says. “Those first 31 patients gave us a look at where we had been and what we would do differently. That has helped with the evolution of the procedure. It’s been vital to decision-making for our patients today.”
Ten years later, Dr. Hoernschemeyer says they can have more educated conversations with families. They have learned more about which patients will benefit most from this surgery and can present more information to help families decide whether to have VBT surgery.
Reflecting on How Far VBT for Scoliosis Has Come
Since Dr. Hoernschemeyer’s first VBT surgery in 2013, the procedure and the technique used to perform it have evolved:
- The first VBT surgery took more than 10 hours to complete. Today, the procedure takes four to five hours.
- The criteria for selecting patients has become more informed and precise, which improves patient outcomes and decreases risk.
- The surgeons who perform VBT surgery are more efficient at properly exposing the spine and closing the incision after the tether is attached.
But even with so much progress, Dr. Hoernschemeyer and his colleagues continue to collect data and study every procedure they perform.
“I look at studying VBT as a responsibility to make sure we are getting better,” Dr. Hoernschemeyer says. “Better at selecting the right patients, better at the procedure itself and achieving better patient outcomes.”
He and his team report that the VBT surgeries they perform preserve motion and anatomy for their patients. In fact, one study found 100% of patients returned to activities like running and biking within the first year of recovery — with nearly 70% of those returns happening within the first three months.
“It’s amazing to see something that didn’t exist in 2000 when I was training as an orthopedic surgeon exist now for the care of kids,” he says. “These types of innovations are changing and revolutionizing care for kids moving forward. And it’s cool to be a part of that.”
Next Steps and Useful Resources
- Want to learn more about VBT? Visit muhealth.org/vbt.